Women’s Health · Emerging Research
Can Mushrooms Help with Period Pain?
New clinical research on a mushroom-derived antioxidant is opening a promising door for natural menstrual relief.
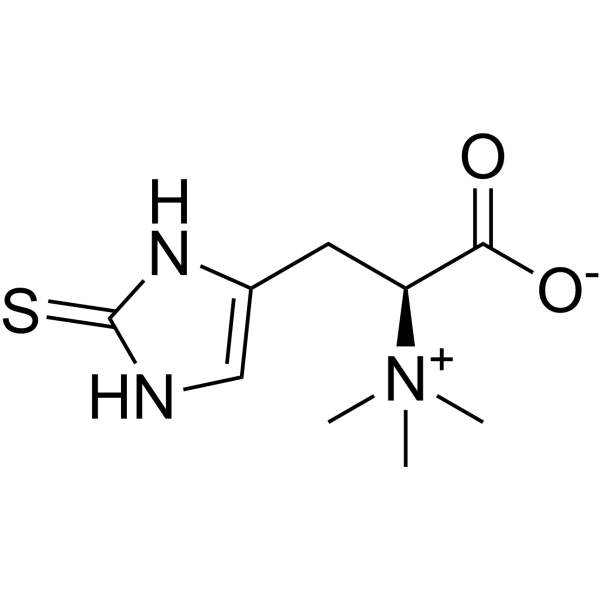
Meet L-Ergothioneine (EGT)
A naturally occurring antioxidant found almost exclusively in fungi, EGT is earning serious attention from researchers. Learn more about ergothioneine →
What Is L-Ergothioneine?
Mushrooms are by far the richest dietary source of EGT — varieties like shiitake, oyster, porcini, and even common white button mushrooms all contain meaningful amounts. What makes EGT remarkable is how the body handles it: humans have a dedicated transporter protein (OCTN1) that actively pulls EGT from food and concentrates it inside cells, particularly in tissues experiencing high oxidative stress. The body essentially flags it as too important to waste.
Once inside cells, EGT scavenges free radicals, protects DNA and proteins from oxidative damage, and helps stabilize mitochondrial function — all at the subcellular level where other antioxidants rarely reach.


Why Oxidative Stress Drives Menstrual Pain
The core driver of primary dysmenorrhea is an overproduction of prostaglandins, which force the uterus to contract intensely — cutting off blood flow and triggering ischemia (oxygen deprivation) in the uterine muscle. That ischemia generates a surge of reactive oxygen species (ROS), unstable molecules that amplify inflammation and pain. Research consistently links elevated oxidative stress with worse cramping severity.
“An antioxidant that concentrates in stressed tissues could interrupt the pain cycle rather than just mask symptoms after the fact.”
If EGT can quench those free radicals inside uterine cells before they fuel the inflammatory cascade, it may offer a fundamentally different approach — acting earlier in the chain, upstream of the pain itself.
What the New Clinical Trial Found

A 2026 randomized, double-blind, placebo-controlled trial enrolled 40 women aged 18–30 with confirmed primary dysmenorrhea. Half received 120 mg/day of oral EGT; the other half received a matching placebo — for three consecutive menstrual cycles. The results were striking.
Equally notable: the benefit was cumulative. A linear mixed model confirmed that EGT’s pain-reducing effect accelerated with each successive cycle — suggesting the compound builds up protective effects over time rather than plateauing. Secondary measures including nausea, fatigue, and mood symptoms (tracked via the COX Menstrual Symptom Scale) also improved significantly. Zero adverse events were reported.
Interestingly, standard serum inflammatory markers (IL-6, TNF-α, PGF2α) didn’t shift significantly between groups, suggesting EGT’s mechanism operates at the intracellular level rather than through classical inflammatory pathways — consistent with how OCTN1-mediated cellular uptake is known to work.
Food vs. Supplements: Getting Enough EGT
Porcini mushrooms contain the highest concentrations of EGT, followed by oyster, shiitake, and maitake. Crucially, EGT is unusually heat-stable — cooking mushrooms doesn’t significantly degrade it. However, reaching the 120 mg/day dose used in the clinical trial from food alone is impractical; a typical serving of shiitake provides only a few milligrams.
For those looking to match clinical trial dosing, a concentrated supplement is the realistic route. Real Mushrooms currently offers one of the only commercially available ergothioneine supplements — providing a reliable, standardized source.
Real Mushrooms Ergothioneine
One of the only commercial sources of concentrated L-ergothioneine supplement available today.
Shop Ergothioneine SupplementExternal link — affiliate relationship disclosed
The Bottom Line
EGT stands out among natural options for period pain because of its distinctive mechanism — targeting oxidative stress at the cellular level, upstream of the pain cascade — and because early human data shows a clinically meaningful effect size. For supplement shoppers looking beyond ibuprofen, it represents one of the more scientifically grounded options to emerge in recent years.
As always, if your pain is severe, worsening, or hasn’t been medically evaluated, see a healthcare provider. Secondary causes of dysmenorrhea like endometriosis require proper diagnosis.
This article is for informational purposes only and does not constitute medical advice. Always consult a qualified healthcare provider before starting any new supplement. The clinical trial referenced is a preprint that has not yet undergone peer review.

No responses yet